Tue, Apr 28, 2026
[Archive]
Volume 11, Issue 4 (Autumn 2025)
JCCNC 2025, 11(4): 283-296 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Jantarapakdee R, Uthis P, Upasen R. Risk Factors of Depression Among Adolescents With Non-suicidal Self-injury: A Systematic Review. JCCNC 2025; 11 (4) :283-296
URL: http://jccnc.iums.ac.ir/article-1-751-en.html
URL: http://jccnc.iums.ac.ir/article-1-751-en.html
1- Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand. & Faculty of Nursing, Burapha University, Chonburi, Thailand.
2- Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand. & Research Unit for Enhancing Well-being in Vulnerable and Chronic Illness Populations, Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand. ,Penpaktr.u@chula.ac.th
3- Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand.
2- Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand. & Research Unit for Enhancing Well-being in Vulnerable and Chronic Illness Populations, Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand. ,
3- Faculty of Nursing, Chulalongkorn University, Bangkok, Thailand.
Keywords: Depression, Self-injurious behavior, Non-suicidal, Risk factors, Adolescent, Systematic review
Full-Text [PDF 838 kb]
(676 Downloads)
| Abstract (HTML) (886 Views)
Study characteristics
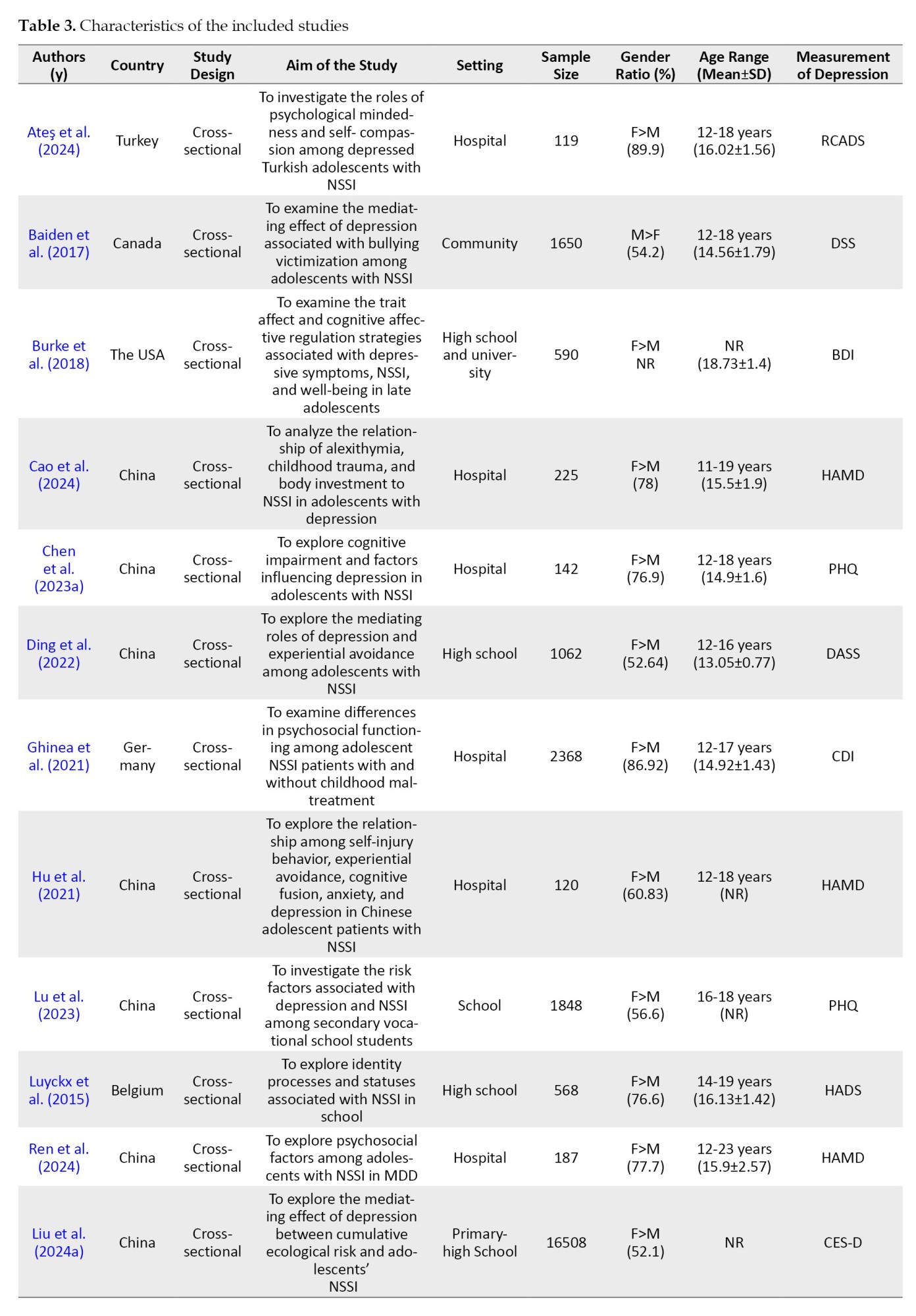
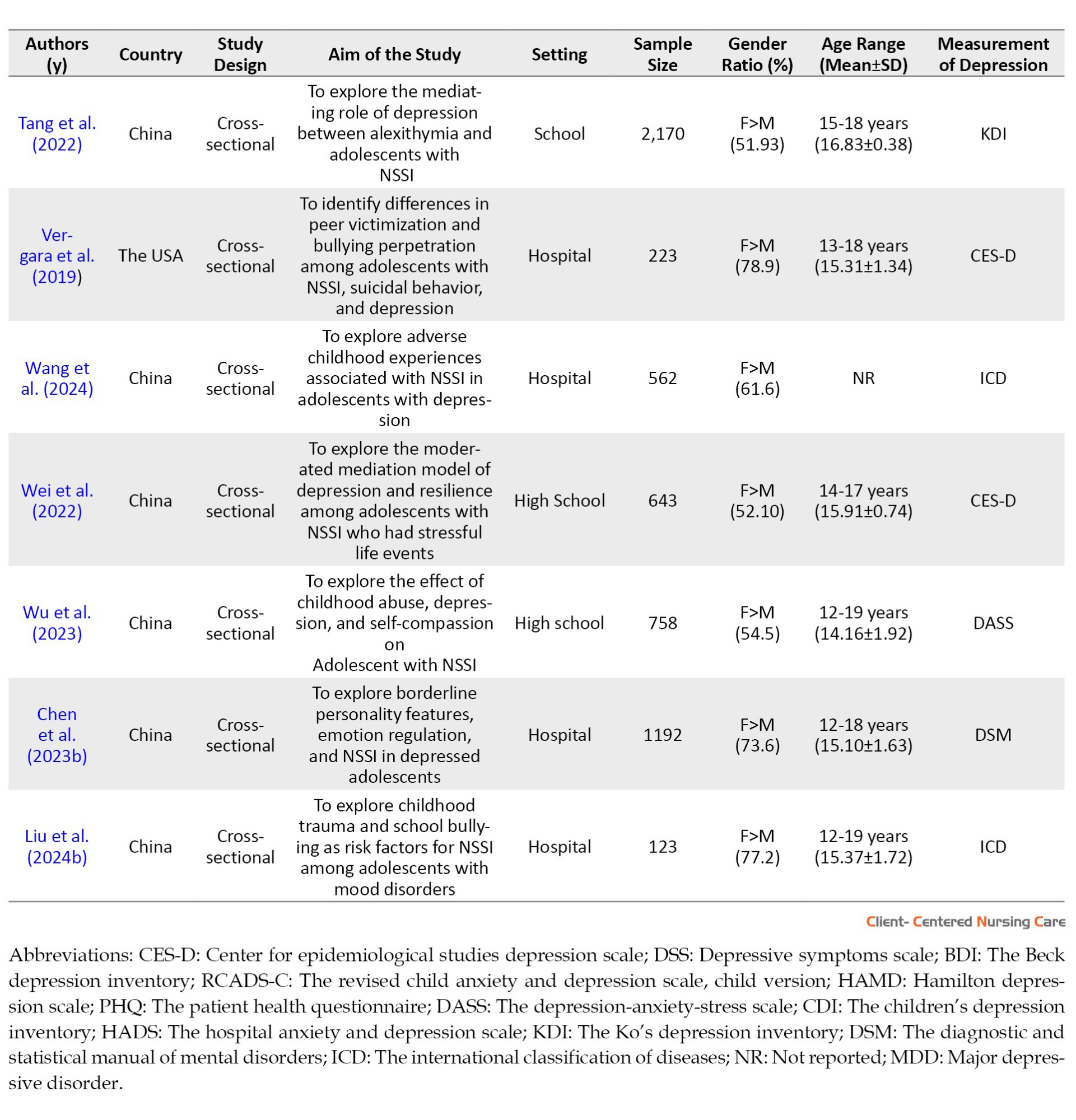
Nineteen studies met the eligibility criteria. All of these were cross-sectional studies; 13 were conducted in China, 2 in the USA, and 1 study each in Canada, Germany, Belgium, and Turkey. The mean age of adolescent participants ranged from 13.05 to 18.73 years, although three studies did not report the mean age of participants. Additionally, ten studies focused on adolescents in hospital settings, while nine involved adolescents in school communities.
The adolescent’s depression had been measured using various measurements, including the Center for epidemiological studies depression scale (CES-D), depressive symptoms scale (DSS), the Beck depression inventory (BDI), the revised child anxiety and depression scale child version (RCADS-C), Hamilton depression scale (HAMD), the patient health questionnaire (PHQ), the depression-anxiety-stress scale (DASS), the children’s depression inventory (CDI), the hospital anxiety and depression scale (HADS), the Ko’s depression inventory (KDI), the diagnostic and statistical manual of mental disorders (DSM), and the international classification of diseases (ICD) (Table 3).
Risk of bias
The Joanna Briggs Institute (JBI) critical appraisal checklist for analytical cross-sectional studies was used to evaluate the methodological quality of eligible studies. This assessment checklist has 8 questions and sections to record answers as “yes,” “no,” “unclear,” or “not applicable” (Moola et al., 2017). All studies were classified as high quality. Of the 19 studies, most described the subjects and settings used valid and reliable measurements and applied appropriate statistical analyses to assess outcomes. However, one study did not describe valid and reliable measures, and six studies did not report confounding factors (Table 4).

Risk factors associated with depression among adolescents with NSSI
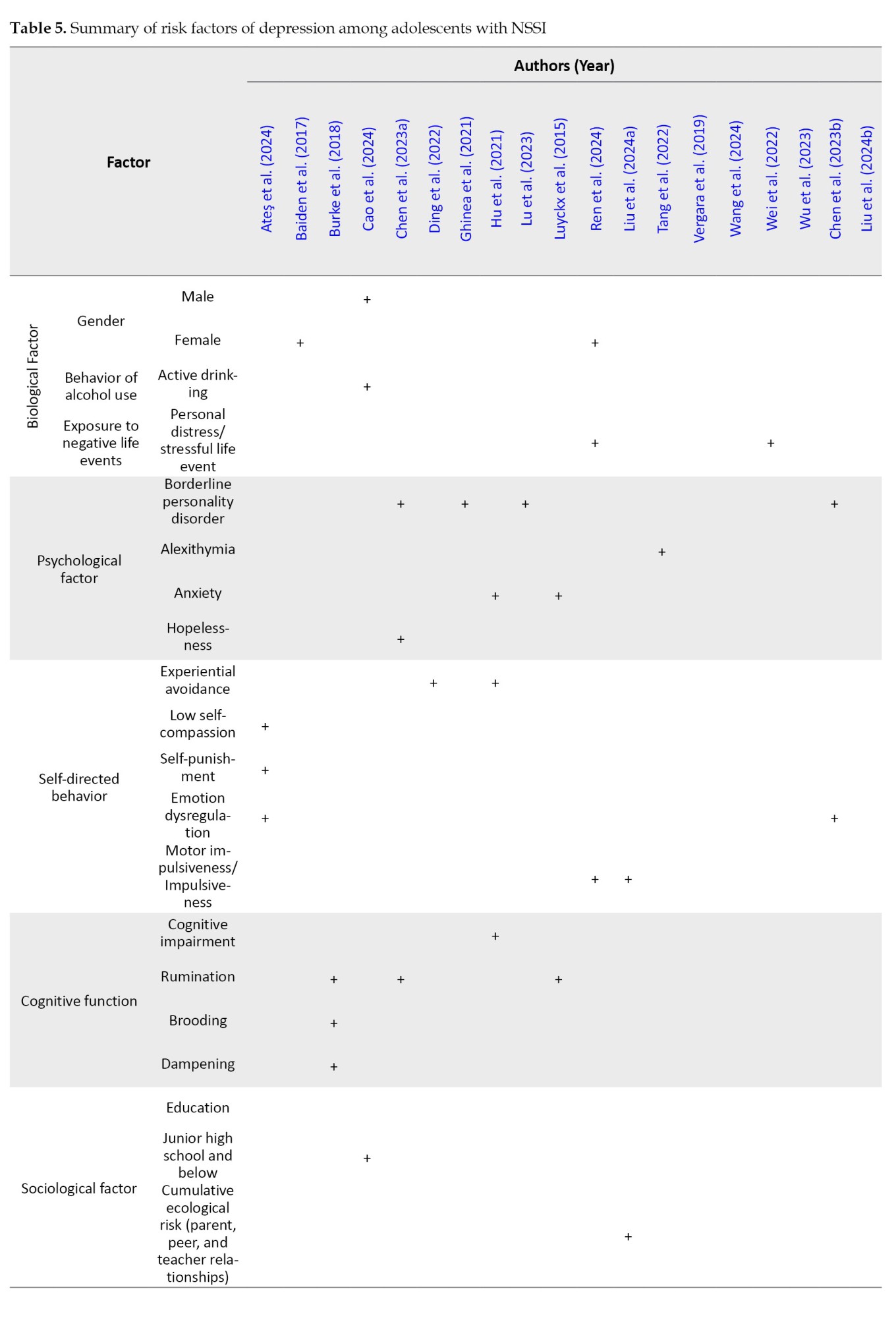
This study found that depression among adolescents with NSSI is influenced by multiple factors, including biological, psychological, and sociological factors (Table 5).
Biological factors
Biological factors encompass fundamental biomedical influences, including genetic predispositions, brain structure and function, and neurochemical imbalances, all of which play a significant role in the development of depression. However, these biological processes can be shaped or exacerbated by external factors such as infections, injuries, diet, exposure to toxins, or trauma, which may impact mental health (Karunamuni et al., 2021). For instance, genetic predispositions may interact with environmental stressors, such as childhood maltreatment or prolonged emotional trauma, increasing the risk of depression and NSSI. These factors can be further explained as follows.
Gender: Out of the 19 studies, two studies reported that being female increases the risk of depression in adolescents with NSSI (Baiden et al., 2017; Ren et al., 2024), while one study reported that being male increases the risk of depression (Cao et al., 2024).
Behavior of alcohol use: Out of the 19 studies, one study indicated that active drinking alcohol use increases the risk of depression (Cao et al., 2024).
Exposure to negative life events: Out of the 19 studies, one indicated that personal distress and stressful life events increased the risk of depression (Wei et al., 2022).
Psychological factors
Psychological factors refer to internal mental processes, emotions, attitudes, and beliefs that influence an individual’s behavior, thoughts, and decision-making (George, 2012). These factors, including coping mechanisms, personality traits, and emotional responses, influence how individuals interact with their environment and experiences. These factors can be explained as follows.
Mental health condition: Out of the 19 studies, four investigated the increased risk of depression among adolescents with borderline personality disorder (Chen et al., 2023a; Chen et al., 2023b; Ghinea et al., 2021; Lu et al., 2023), while two studies indicated that anxiety also raises the risk of depression (Hu et al., 2021; Luyckx et al., 2015). Additionally, one study found that alexithymia increases the risk of depression (Tang et al., 2022), and another found that hopelessness increases the risk of depression (Chen et al., 2023a).
Self-directed behaviors: Out of the 19 studies, two investigated that experiential avoidance increased the risk of depression (Ding et al., 2022; Hu et al., 2021), while two studies indicated that emotion dysregulation also raises the risk of depression (Ateş et al., 2024; Chen et al., 2023b). Additionally, two indicated that impulsiveness also increases the risk of depression (Liu et al., 2024; Ren et al., 2024), and another indicated that low self-compassion and self-punishment increase the risk of depression (Ateş et al., 2024).
Cognitive function: Out of the 19 studies, three investigated rumination through increased risk of depression, including brooding and dampening (Burke et al., 2018; Chen et al., 2023a; Luyckx et al., 2015), while one study reported cognitive impairment increased risk of depression (Hu et al., 2021).
Sociological factors
Sociological factors refer to the societal and environmental aspects that shape human behavior, beliefs, and interactions (George, 2012). These factors encompass social structures, cultural norms, and systemic elements, including family, religion, education, socioeconomic status, and community values. These factors can be explained as follows.
Education: Out of the 19 studies, one indicated that adolescents in junior high school or below have an increased risk of depression (Cao et al., 2024).
Cumulative ecological risk: Only one of the 19 studies examined cumulative ecological factors that predicted depression in adolescents with NSSI, including connections between parents and children, peers, and teachers and students (Liu et al., 2024).
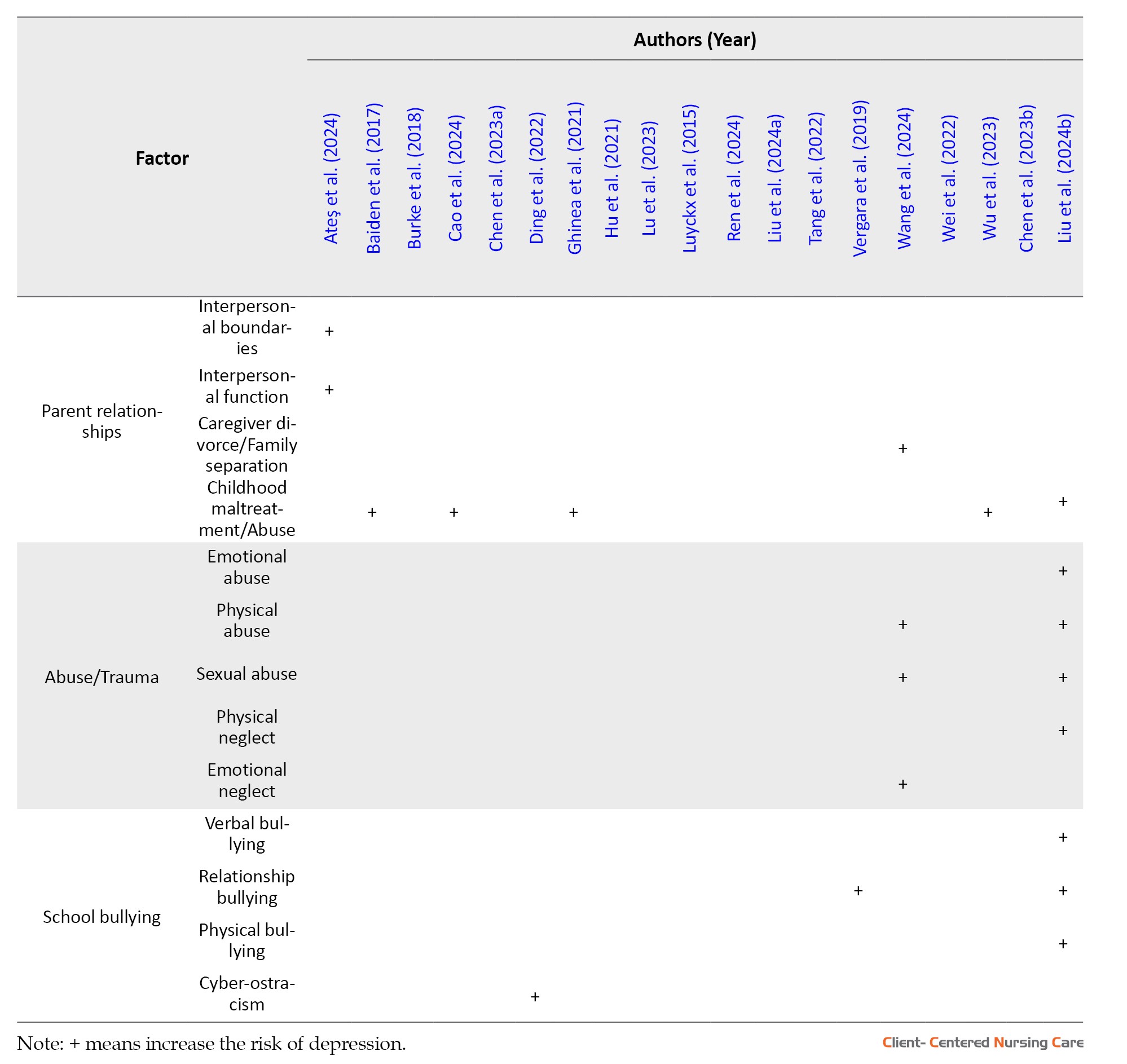
Parent relationships: Out of the 19 studies, 5 studies reported that childhood maltreatment or childhood abuse increases the risk of depression (Baiden et al., 2017; Cao et al., 2024; Ghinea et al., 2021; Liu et al., 2024b; Wu et al., 2023). Additionally, one study indicated that caregiver divorce or family separation increases the risk of depression (Wang et al., 2024), and another indicated that interpersonal boundaries and function increase the risk of depression (Ateş et al., 2024).
Abuse/Trauma: Out of the 19 studies, two studies reported that physical and sexual abuse increase the risk of depression (Liu et al., 2024b; Wang et al., 2024). Additionally, one study investigated that emotional neglect increases the risk of depression (Wang et al., 2024), and another identified that emotional abuse and physical neglect increase the risk of depression (Liu et al., 2024b).
School bullying: Out of the 19 studies, three studies indicated that relationship bullying increases the risk of depression (Liu et al., 2024b; Vergara et al., 2019; Wang et al., 2024), while one study identified that cyber-ostracism increases the risk of depression (Ding et al., 2022). Additionally, one study investigated how verbal and physical bullying increases the risk of depression (Liu et al., 2024b).
Discussion
This systematic review explored risk factors associated with depression in adolescents who engage in NSSI. A total of 19 cross-sectional studies among 31058 adolescents with NSSI met the eligibility criteria. The findings indicated that depression risk is influenced by three key domains: Biological factors, including female gender, behavior of alcohol use, and exposure to negative life events; psychological factors, such as pre-existing mental health conditions, psychological distress, and cognitive functioning; and sociological factors, including educational background, parental relationships, experiences of abuse or trauma, and peer bullying. These findings highlight the multifaceted nature of depression risk in this population.
Biological factors
The literature reports that women, in particular, who engage in NSSI are more likely than men to have experienced depression (Baiden et al., 2017; Ren et al., 2024). However, one study reported that being male gender increases the risk of depression (Cao et al., 2024). The reason for the gender differences may be related to the fact that women generally have higher rates of depression and anxiety than men (Hilt et al., 2008). The average age of adolescent participants ranged from 13.05 to 18.73 years. The finding was consistent with the previous review by Cao et al. (2024), who indicated that adolescents in junior high school or below have an increased risk of depression. Similarly, Kessler et al. (2005) explained that mid-adolescent age is a predictor of NSSI across the lifespan, as adolescence is a critical period for human development in lifelong well-being. Still, the risk of poor mental health is found in 50% of all mental disorders beginning by age 14. Moreover, adolescents experiencing personal distress and stressful life events have an increased risk of depression (Ren et al., 2024; Wei et al., 2022). This finding is consistent with the findings of Baetens et al. (2021), who reported that the presence of depression in adolescents with NSSI is associated with an increased likelihood of experiencing stressful life events. Adolescents engaging in NSSI may be more susceptible to interpersonal conflicts, including arguments with parents, teachers, friends, or romantic partners. Additionally, these findings align with previous research suggesting that depression may serve as a mechanism linking stressful life events to NSSI in adolescents (Burke et al., 2015; Liu et al., 2021).
Psychological factors
This review found that psychological factors are strongly associated with depression in adolescents with NSSI, which is often used to regulate distressing emotions, manage stress, or self-punishment. It may also serve as an outlet for self-directed anger, self-blame, and perceived social transgressions (Chapman & Dixon-Gordon, 2007; Klonsky & Muehlenkamp, 2007). Additionally, mental health condition increases the risk of depression, such as borderline personality disorder, anxiety, alexithymia, and hopelessness (Chen et al., 2023a; Chen et al., 2023b; Ghinea et al., 2021; Hu et al., 2021; Lu et al., 2023; Luyckx et al., 2015; Tang et al., 2022). The findings align with previous studies that highlighted how depression among adolescents with NSSI may be linked to other mental health conditions, particularly in those who struggle with mood regulation (Andover & Gibb, 2010; Whitlock et al., 2014). NSSI is often carried out as an attempt to avoid interpersonal interactions. Individuals with mood disorders who engage in NSSI frequently have a history of poor or negative relationships, exhibit impulsiveness, and experience low self-compassion, which may also engage in self-punishment, as shown in previous findings.
Cognitive function, including rumination thought, brooding, dampening, and cognitive impairment, is associated with depression (Burke et al., 2018; Chen et al., 2023a; Hu et al., 2021; Luyckx et al., 2015). The response style theory developed by Nolen-Hoeksema (1991) explains that an individual’s response to distractions can lead to depression, particularly in those with a tendency to ruminate. Rumination involves repetitive, negative thoughts that prolong distress and increase the risk of depression more than in individuals who do not engage in such thinking patterns.
Sociological factors
The findings highlight cumulative ecological risks, including poor parent-child relationships, adverse family life events, academic challenges, teacher-student relationships, and peer relationships (Liu et al., 2024a). Sociological factors, including parent relationships, abuse, and school bullying, were identified as risk factors for depression. This systematic review indicates that childhood maltreatment or abuse, caregiver divorce or family separation, and interpersonal boundary issues increase the risk of depression (Ateş et al., 2024; Baiden et al., 2017; Cao et al., 2024; Ghinea et al., 2021; Liu et al., 2024b; Wang et al., 2024; Wu et al., 2023). This finding may be because childhood abuse is often associated with long-term emotional dysfunction. Adolescents with a history of childhood abuse tend to struggle with affect and emotion regulation and may experience a sense of insecurity, which can consequently lead to NSSI (Santangelo et al., 2016).
Moreover, being abused from childhood trauma such as physical abuse, sexual abuse, emotional abuse, emotional neglect, and physical neglect is a risk factor for depression (Liu et al., 2024b; Wang et al., 2024). It suggests that victims of sexual abuse often experience a profound sense of betrayal and depersonalization, which can lead to maladaptive strategies for regulating emotions in an attempt to reduce emotional distress (Lu et al., 2023). Moreover, physical abuse significantly affects adolescents with depression who engage in NSSI, as these adolescents often have limited emotion regulation skills. The negative emotions stemming from physical abuse may lead them to use NSSI as a quick way to regulate their emotions (Chapman & Dixon-Gordon, 2007). These findings confirm that a sense of loss and helplessness when witnessing caregivers being treated violently contribute to various mental health issues, such as depression, which were identified as predictors of NSSI.
School bullying by peers, such as relationship bullying, cyber-ostracism, and verbal and physical bullying, is found to be a risk factor for depression (Ding et al., 2022; Liu et al., 2024b; Wang et al., 2024). This finding suggests that experiencing school bullying can be a significant stressor that leads to an accumulation of depression, potentially resulting in self-injurious behavior as a form of emotional relief (Ford & Gómez, 2015). Similarly, adolescents who are victims of school bullying may experience depression and engage in self-harm as a coping mechanism or form of self-punishment (Nguyen et al., 2020).
This study has some limitations. The inclusion criteria are limited to English-language publications from 2014 to 2024, which may introduce selection bias. Furthermore, some studies did not provide the average age of participants, which could potentially impact the results, as adolescence is divided into three stages: Early, middle, and late adolescence, each with distinct developmental characteristics. Specifying the average age could help clarify which stage of adolescence is most associated with NSSI and an increased risk of developing depression. Moreover, the measurement of depression differed among studies, with some using a wide range of scores that might also include other disorders such as anxiety and stress. This may lead to variability in measuring depression due to the influence of comorbid conditions.
Conclusion
The findings are classified into three categories of factors associated with depression among adolescents with NSSI. These are biological factors, consisting of gender, behavior of alcohol use, and exposure to negative life events; psychological factors, consisting of mental health conditions, psychological behaviors, and cognitive function; and sociological factors, consisting of education, parent relationships, experiences of abuse or trauma, and school bullying.
Ethical Considerations
Compliance with ethical guidelines
The study protocol was registered with the international prospective register of systematic reviews (PROSPERO) (Code: CRD42024555723).
Funding
This study was extracted from the PhD dissertation of Russunan Jantarapakdee, approved by the Faculty of Nursing at Chulalongkorn University, Bangkok, Thailand. This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Investigation, data collection, and validation: Russunan Jantarapakdee and Ratchaneekorn Upasen; Data analysis and writing: Russunan Jantarapakdee and Penpaktr Uthis; Final approval: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors want to express their gratitude to the Faculty of Nursing, Chulalongkorn University and the Faculty of Nursing, Burapha University for providing their constant support for the study.
References
American Academy of Pediatrics., 2019. Stages of adolescence. Illinois: American Academy of Pediatrics. [Link]
Andover, M. S. & Gibb, B. E., 2010. Non-suicidal self-injury, attempted suicide, and suicidal intent among psychiatric inpatients. Psychiatry Research, 178(1), pp. 101-5. [DOI:10.1016/j.psychres.2010.03.019] [PMID]
Asarnow, J. R., et al., 2011. Suicide attempts and nonsuicidal self-injury in the treatment of resistant depression in adolescents: Findings from the TORDIA study. Journal of the American Academy of Child and Adolescent Psychiatry, 50(8), pp. 772–81.[DOI:10.1016/j.jaac.2011.04.003] [PMID]
Ateş, B. Ö., et al., 2024. Self-compassion and psychological mindedness in depressed Turkish adolescents with non-suicidal self-injury. Australian Psychologist, 59(5), pp. 435-48. [DOI:10.1080/00050067.2024.2371802]
Baetens, I., et al., 2021. Predictors and consequences of non-suicidal self-injury in relation to life, peer, and school factors. Journal of Adolescence, 90, pp. 100–8. [DOI:10.1016/j.adolescence.2021.06.005] [PMID]
Baiden, P., Stewart, S. L. & Fallon, B., 2017. The mediating effect of depressive symptoms on the relationship between bullying victimization and non-suicidal self-injury among adolescents: Findings from community and inpatient mental health settings in Ontario, Canada. Psychiatry Research, 255, pp. 238–47. [DOI:10.1016/j.psychres.2017.05.018] [PMID]
Barrocas, A. L., et al., 2015. Nonsuicidal self-injury in adolescence: Longitudinal course, trajectories, and intrapersonal predictors. Journal of Abnormal Child Psychology, 43(2), pp. 369–80. [DOI:10.1007/s10802-014-9895-4] [PMID]
Bousoño, M., et al., 2021. Alcohol use and risk factors for self-harm behavior in Spanish adolescents. Adicciones, 33(1), pp. 53–62. [DOI:10.20882/adicciones.1239] [PMID]
Bronfenbrenner, U., 2005. Making human beings human: Bioecological perspectives on human development. California: SAGE. [Link]
Brown, R. C. & Plener, P. L., 2017. Non-suicidal Self-Injury in Adolescence. Current Psychiatry Reports, 19(3), pp. 20. [DOI:10.1007/s11920-017-0767-9] [PMID]
Burke, T. A., et al., 2018. Latent classes of trait affect and cognitive affective regulation strategies are associated with depression, non-suicidal self-injury, and well-being. Journal of Affective Disorders, 225, pp. 180–7. [DOI:10.1016/j.jad.2017.08.015] [PMID]
Burke, T. A., et al., 2015. Non-suicidal self-injury prospectively predicts interpersonal stressful life events and depressive symptoms among adolescent girls. Psychiatry Research, 228(3), pp.416–24. [DOI:10.1016/j.psychres.2015.06.021] [PMID]
Cao, P., et al., 2024. Predictors of non-suicidal self-injury in adolescents with depressive disorder: the role of alexithymia, childhood trauma, and body investment. Frontiers in Psychology, 15, pp. 1336631. [DOI:10.3389/fpsyg.2024.1336631] [PMID]
Chapman, A. & Dixon-Gordon, K., 2007. Emotional antecedents and consequences of deliberate self-harm and suicide attempts. Suicide & Life-Threatening Behavior, 37(5), pp. 543–52. [DOI:10.1521/suli.2007.37.5.543] [PMID]
Chen, H., et al., 2023. Cognitive impairment and factors influencing depression in adolescents with suicidal and self-injury behaviors: A cross-sectional study. BMC Psychiatry, 23(1), pp. 247. [DOI:10.1186/s12888-023-04726-8] [PMID]
Chen, Y., et al., 2023. Relationship between borderline personality features, emotion regulation, and non-suicidal self-injury in depressed adolescents: A cross-sectional study. BMC Psychiatry, 23(1), pp. 293. [DOI:10.1186/s12888-023-04800-1] [PMID]
Claes, L., et al., 2010. Comparison of non-suicidal self-injurious behavior and suicide attempts in patients admitted to a psychiatric crisis unit. Personality and Individual Differences, 48(1), pp. 83-7. [DOI:10.1016/j.paid.2009.09.001]
Ding, H., et al., 2022. The relationship between cyber-ostracism and adolescents’ non-suicidal self-injury: Mediating roles of depression and experiential avoidance. International Journal of Environmental Research and Public Health, 19(19), pp. 12236. [DOI:10.3390/ijerph191912236] [PMID]
Du, N., et al., 2021. Psychosocial factors associated with increased adolescent non-suicidal self-injury during the covid-19 pandemic. Frontiers in Psychiatry, 12, pp. 743526. [DOI:10.3389/fpsyt.2021.743526] [PMID]
Esposito, C., et al., 2023. Prevalence of engagement and frequency of non-suicidal self-injury behaviors in adolescence: An investigation of the longitudinal course and the role of temperamental effortful control. European Child & Adolescent Psychiatry, 32(12), pp. 2399–414. [DOI:10.1007/s00787-022-02083-7] [PMID]
Ford, J. D. & Gómez, J. M., 2015. The relationship of psychological trauma and dissociative and posttraumatic stress disorders to nonsuicidal self-injury and suicidality: A review. Journal of Trauma & Dissociation: The Official Journal of the International Society for the Study of Dissociation (ISSD), 16(3), pp. 232–71. [DOI:10.1080/15299732.2015.989563] [PMID]
George, L. E., 2012. The need for a new medical model: A challenge for biomedicine. Psychodynamic Psychiatry, 40(3), pp. 377-96. [DOI:10.1521/pdps.2012.40.3.377] [PMID]
Ghinea, D., et al., 2021. Psychosocial functioning in adolescents with non-suicidal self-injury: the roles of childhood maltreatment, borderline personality disorder and depression. Borderline Personality Disorder and Emotion Dysregulation, 8(1), pp. 21. [DOI:10.1186/s40479-021-00161-x] [PMID]
Gillies, D., et al., 2018. Prevalence and characteristics of self-harm in adolescents: Meta-Analyses of community-based studies 1990-2015. Journal of the American Academy of Child and Adolescent Psychiatry, 57(10), pp. 733–41. [DOI:10.1016/j.jaac.2018.06.018] [PMID]
Hilt, L. M., Cha, C. B. & Nolen-Hoeksema, S., 2008. Nonsuicidal self-injury in young adolescent girls: Moderators of the distress-function relationship. Journal of Consulting and Clinical Psychology, 76(1), pp. 63–71. [DOI:10.1037/0022-006X.76.1.63] [PMID]
Hu, Z., et al., 2021. Relationship among self-injury, experiential avoidance, cognitive fusion, anxiety, and depression in Chinese adolescent patients with nonsuicidal self-injury. Brain and Behavior, 11(12), pp. e2419. [DOI:10.1002/brb3.2419] [PMID]
Jin, M. K., et al., 2023. A systematic review and meta-analysis of factors related to non-suicidal self-injury among Chinese adolescents. Psychiatry Research, 326, pp. 115329. [DOI:10.1016/j.psychres.2023.115329] [PMID]
Kabkumba, C., Kaewjanta, N., & Rungreangkulkij, S. (2021). Non-suicidal self-harm behaviour and risk factors amongst undergraduate nursing students. Journal of Thailand Nursing and Midwifery Council 37(1), 146-160. [Link]
Karunamuni, N., Imayama, I. & Goonetilleke, D., 2021. Pathways to well-being: Untangling the causal relationships among biopsychosocial variables. Social Science & Medicine (1982), 272, pp. 112846. [DOI:10.1016/j.socscimed.2020.112846] [PMID]
Kerr, P. L., Muehlenkamp, J. J. & Turner, J. M., 2010. Nonsuicidal self-injury: A review of current research for family medicine and primary care physicians. Journal of the American Board of Family Medicine: JABFM, 23(2), pp. 240–59. [DOI:10.3122/jabfm.2010.02.090110] [PMID]
Kessler, R. C., et al., 2005. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry, 62(6), pp. 593-602. [DOI:10.1001/archpsyc.62.6.593] [PMID]
Klonsky, E. D. & Muehlenkamp, J. J., 2007. Self-injury: A research review for the practitioner. Journal of Clinical Psychology, 63(11), pp. 1045–56. [DOI:10.1002/jclp.20412] [PMID]
Lawrence, D., et al., 2016. Key findings from the second Australian Child and Adolescent Survey of Mental Health and Wellbeing. The Australian and New Zealand Journal of Psychiatry, 50(9), pp. 876–86. [DOI:10.1177/0004867415617836] [PMID]
Liu, S., et al., 2024. Cumulative ecological risk and nonsuicidal self-injury in adolescents: The mediation of depression and the moderation of impulsiveness. Child: Care, Health and Development, 50(1), pp. e13211. [DOI:10.1111/cch.13211] [PMID]
Liu, Y., et al., 2024. The mediating effects of school bullying victimization in the relationship between childhood trauma and NSSI among adolescents with mood disorders. BMC Pediatrics, 24(1), pp. 524. [DOI:10.1186/s12887-024-04986-7] [PMID]
Liu, Z. Z., et al., 2021. Depression as a mediator between frequent nightmares and non-suicidal self-injury among adolescents: A 3-wave longitudinal model. Sleep Medicine, 77, pp. 29–34. [DOI:10.1016/j.sleep.2020.11.015] [PMID]
Lu, Z., et al., 2023. The relationship between depressive mood and non-suicidal self-injury among secondary vocational school students: The moderating role of borderline personality disorder tendencies. Frontiers in Psychiatry, 14, pp. 1187800.[DOI:10.3389/fpsyt.2023.1187800] [PMID]
Luyckx, K., et al., 2015. Non-suicidal self-injury in high school students: Associations with identity processes and statuses. Journal of Adolescence, 41, pp.76–85. [DOI:10.1016/j.adolescence.2015.03.003] [PMID]
Moola S, et al., 2017. Chapter 7: Systematic reviews of etiology and risk. In: Aromataris E, Munn Z (Editors). Checklist for analytical. Cross sectional studies. North Adelaide: The Joanna Briggs Institute. [Link]
Moola, S., et al., 2020. Systematic reviews of etiology and risk.In: E. Aromataris & Z. Munn (Editors). JBI Manual for Evidence Synthesis. Adelaide: JBI. [Link]
Muehlenkamp, J. J. & Brausch, A. M., 2019. Protective factors do not moderate risk for past-year suicide attempts conferred by recent NSSI. Journal of Affective Disorders, 245, pp. 321–4. [DOI:10.1016/j.jad.2018.11.013] [PMID]
Nguyen, H. T. L., et al., 2020. Relationships among cyberbullying, parental attitudes, self-harm and suicidal behavior among adolescents: Results from a school-based survey in Vietnam. BMC Public Health, 20(1), pp. 476. [DOI:10.1186/s12889-020-08500-3] [PMID]
Nolen-Hoeksema, S., 1991. Responses to depression and their effects on the duration of depressive episodes. Journal of Abnormal Psychology, 100(4), pp. 569–82. [DOI:10.1037/0021-843X.100.4.569] [PMID]
Page, M. J., et al., 2021. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ (Clinical research ed.), 372, pp. n71. [PMID]
Ren, T., et al., 2024. Psychosocial factors affect the occurrence of nonsuicidal self-injury in adolescents with major depressive disorder through chain mediation. European Archives of Psychiatry and Clinical Neuroscience, 275(4), pp. 1209–20.[DOI:10.1007/s00406-024-01858-0] [PMID]
Santangelo, P. S., et al., 2017. Ecological momentary assessment of affective and interpersonal instability in adolescent non-suicidal self-injury. Journal of Abnormal Child Psychology, 45(7), pp. 1429–38. [DOI:10.1007/s10802-016-0249-2] [PMID]
Shao, C., et al., 2021. Analysis of risk factors of non-suicidal self-harm behavior in adolescents with depression. Annals of Palliative Medicine, 10(9), pp. 9607–13. [DOI:10.21037/apm-21-1951] [PMID]
Tang, W. C., et al., 2022. Mediating role of depression in the association between alexithymia and nonsuicidal self-injury in a representative sample of adolescents in Taiwan. Child and Adolescent Psychiatry and Mental Health, 16(1), pp. 43. [DOI:10.1186/s13034-022-00477-8] [PMID]
Thai, T. T., et al., 2021.The prevalence, correlates and functions of non-suicidal self-injury in Vietnamese adolescents. Psychology Research and Behavior Management, 14, pp. 1915–27. [DOI:10.2147/PRBM.S339168] [PMID]
Vergara, G. A., et al., 2019. Non-Suicidal self-injury and suicide in depressed Adolescents: Impact of peer victimization and bullying. Journal of Affective Disorders, 245, pp. 744–9. [DOI:10.1016/j.jad.2018.11.084] [PMID]
Wang, L., et al., 2024. Prevalence of adverse childhood experiences and their associations with non-suicidal self-injury among Chinese adolescents with depression. Child Psychiatry and Human Development, 55(5), pp. 1441–51. [DOI:10.1007/s10578-023-01508-x] [PMID]
Wang, Y. J., et al., 2022. Risk factors for non-suicidal self-injury (NSSI) in adolescents: A meta-analysis. EClinicalMedicine, 46, pp. 101350. [DOI:10.1016/j.eclinm.2022.101350] [PMID]
Wei, C., et al., 2022. Stressful life events and non-suicidal self-injury among Chinese adolescents: A moderated mediation model of depression and resilience. Frontiers in Public Health, 10, pp. 944726. [DOI:10.3389/fpubh.2022.944726] [PMID]
Whitlock, J., Exner-Cortens, D. & Purington, A., 2014. Assessment of nonsuicidal self-injury: Development and initial validation of the Non-Suicidal Self-Injury-Assessment Tool (NSSIAT). Psychological Assessment, 26(3), pp. 935–46. [DOI:10.1037/a0036611] [PMID]
Wu, J., et al., 2023. The effects of childhood abuse, depression, and self-compassion on adolescent nonsuicidal self-injury: A moderated mediation model. Child Abuse & Neglect, 136, pp. 105993. [DOI:10.1016/j.chiabu.2022.105993] [PMID]
Yu, L., et al., 2023. Multicenter analysis on the non-suicidal self-injury behaviors and related influencing factors-A case study of left-behind children in northeastern Sichuan. Journal of Affective Disorders, 320, pp. 161–8. [DOI:10.1016/j.jad.2022.09.081] [PMID]
Full-Text: (411 Views)
Introduction
Non-suicidal self-injury (NSSI) is a self-directed action that leads to direct, deliberate destruction or alteration of one’s bodily tissue without suicidal intent (Kerr et al., 2010; Muehlenkamp & Brausch, 2019). NSSI is widely recognized as an emotional self-regulation strategy, primarily used to relieve intense negative emotions such as stress, anxiety, depression, anger, and frustration. These emotions typically precede NSSI and are often followed by a temporary sense of relief or calm (Klonsky & Muehlenkamp, 2007).
NSSI typically begins in early adolescence, with the mean onset age of 13 years (Gillies et al., 2018), and emerges during early to middle adolescence, reaching its peak around the ages of 14-15, then gradually declines during late adolescence (Esposito et al., 2023). Previous studies report that NSSI affects 13%–29% of adolescents (Baetens et al., 2021; Muehlenkamp & Brausch, 2019). It is a significant mental health concern in the community and clinical settings, with lifetime prevalence estimates ranging from 17% to 60% (Brown & Plener, 2017). Additionally, depression is highly prevalent among adolescents who engage in NSSI (Barrocas et al., 2015; Kabkumba et al., 2021; Lawrence et al., 2016; Shao et al., 2021; Thai et al., 2021). Depression in adolescents with NSSI can elevate the risk of suicide when they struggle to cope with negative emotions, as recent studies indicate that those with depression exhibit significantly higher levels of suicidal ideation, attempts, and predicted suicidal behavior over time (Asarnow et al., 2011; Bousoño et al., 2021; Chapman & Dixon-Gordon, 2007; Claes et al., 2010; Thai et al., 2021; Yu et al., 2023).
Currently, numerous studies have investigated the risk factors associated with NSSI among adolescents (Brown & Plener, 2017; Du et al., 2021; Thai et al., 2021). Additionally, systematic reviews and meta-analyses have been conducted to examine factors associated with NSSI in adolescents (Jin et al., 2023; Wang et al., 2022). While NSSI has multiple risk factors, depression may serve as a mediator that intensifies or prolongs NSSI behaviors. Identifying the risk factors contributing to depression in adolescents with NSSI can help both researchers and practitioners develop more effective, tailored interventions. To address this gap, we conducted a systematic review to identify the risk factors of depression among adolescents with NSSI that could be utilized to develop interventions that reduce risk factors leading to depression in NSSI.
Material and Methods
Search strategy
Searching was conducted across four databases, consisting of PubMed, CINAHL, ScienceDirect, and Scopus, from 2014 to 2024. Limiting the review to the past
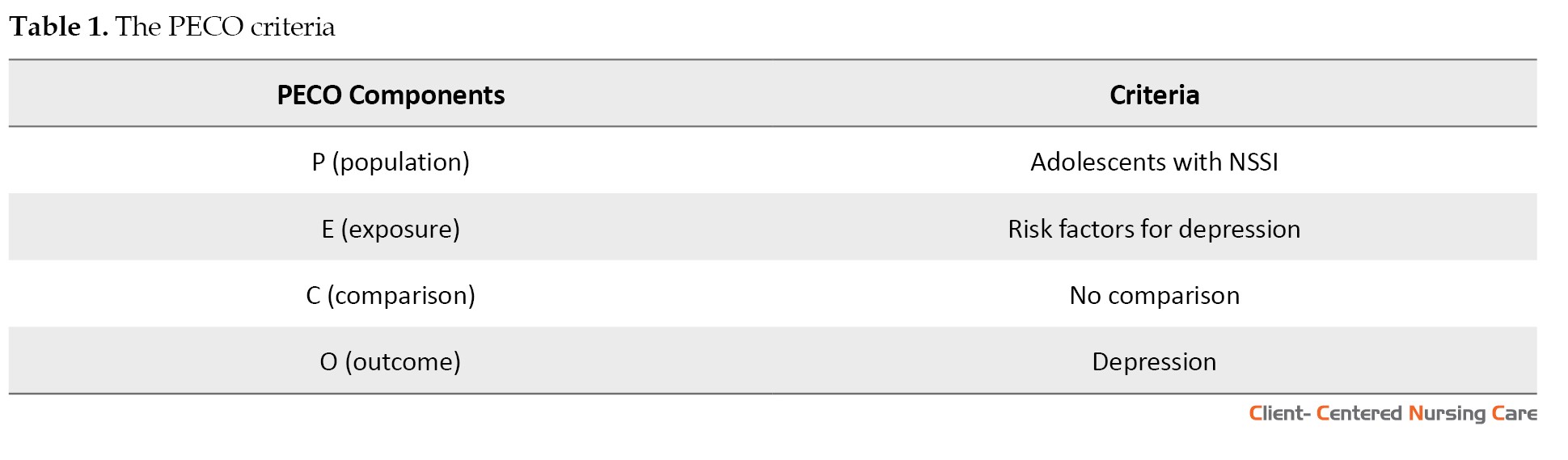
decade ensures that our findings are based on the most up-to-date evidence. We performed a systematic review of the literature, which followed the preferred reporting items for systematic reviews and meta-analysis (PRISMA) guidelines outlined in (Page et al., 2021). We aimed to answer the PECO criteria to formulate a focused review question, “What are the risk factors for depression among adolescents with NSSI?” (Table 1).
All retrieved articles were imported into EndNote software, version 21 to identify relevant studies and remove duplicates. We used boolean operators (AND, OR, NOT, or AND NOT) as conjunctions to combine or exclude keywords in our searching (Table 2).

Eligibility criteria and study selection
The study population is adolescents with NSSI who are 10-21 years old and presented with depression (American Academy of Pediatrics, 2019). No specific intervention was required for inclusion in this review. Studies relevant to non-experimental designs, such as cross-sectional studies, published in English between 2014 and 2024, were included. However, studies were excluded if they were not available in full text, if the sample populations consisted of adults or older people, or if they were case studies, systematic reviews, or meta-analysis articles.
Data extraction and synthesis
Data extraction and cross-checking were conducted by two authors, who screened the articles by reviewing their design, participants, risk factors, measurements, and main findings to determine if they met the inclusion criteria. After this screening procedure, full-text articles were analyzed in detail for final inclusion, focusing on the relationship between depression and its associated factors. Data were summarized as adjusted odds ratios, and multivariate findings took precedence over unadjusted odds ratios and bivariate results. Any disagreements between the two authors were referred to a third author for a final decision. We conducted a narrative synthesis to identify risk factors of depression. We categorized findings of the included studies into three domains (biological, psychological, and sociological factors), enabling us to identify common risk factors for depression and inconsistencies across studies. To enhance clarity, we developed a summary table to present findings in a structured format.
Quality assessment
The quality of the studies was assessed by using the Joanna Briggs Institute (JBI) critical appraisal checklist (Moola et al., 2020) for cross-sectional studies. Studies scoring over 70% (6–8 points) were classified as high quality, those scoring between 50% and 70% (4–5 points) as medium quality, and those below 50% (below 4 points) as low quality (Moola et al., 2017).
Results
Following the selection process, 2457 articles were imported into EndNote software, to identify relevant articles and remove duplicates (1431 articles). This process left 1026 potentially relevant sources. Of these, 1007 articles were excluded for various reasons, such as lack of full text, not focusing on adolescents, or being related to other diseases. Finally, 19 articles were selected that satisfied the criteria set forth for this systematic review (Figure 1).
Non-suicidal self-injury (NSSI) is a self-directed action that leads to direct, deliberate destruction or alteration of one’s bodily tissue without suicidal intent (Kerr et al., 2010; Muehlenkamp & Brausch, 2019). NSSI is widely recognized as an emotional self-regulation strategy, primarily used to relieve intense negative emotions such as stress, anxiety, depression, anger, and frustration. These emotions typically precede NSSI and are often followed by a temporary sense of relief or calm (Klonsky & Muehlenkamp, 2007).
NSSI typically begins in early adolescence, with the mean onset age of 13 years (Gillies et al., 2018), and emerges during early to middle adolescence, reaching its peak around the ages of 14-15, then gradually declines during late adolescence (Esposito et al., 2023). Previous studies report that NSSI affects 13%–29% of adolescents (Baetens et al., 2021; Muehlenkamp & Brausch, 2019). It is a significant mental health concern in the community and clinical settings, with lifetime prevalence estimates ranging from 17% to 60% (Brown & Plener, 2017). Additionally, depression is highly prevalent among adolescents who engage in NSSI (Barrocas et al., 2015; Kabkumba et al., 2021; Lawrence et al., 2016; Shao et al., 2021; Thai et al., 2021). Depression in adolescents with NSSI can elevate the risk of suicide when they struggle to cope with negative emotions, as recent studies indicate that those with depression exhibit significantly higher levels of suicidal ideation, attempts, and predicted suicidal behavior over time (Asarnow et al., 2011; Bousoño et al., 2021; Chapman & Dixon-Gordon, 2007; Claes et al., 2010; Thai et al., 2021; Yu et al., 2023).
Currently, numerous studies have investigated the risk factors associated with NSSI among adolescents (Brown & Plener, 2017; Du et al., 2021; Thai et al., 2021). Additionally, systematic reviews and meta-analyses have been conducted to examine factors associated with NSSI in adolescents (Jin et al., 2023; Wang et al., 2022). While NSSI has multiple risk factors, depression may serve as a mediator that intensifies or prolongs NSSI behaviors. Identifying the risk factors contributing to depression in adolescents with NSSI can help both researchers and practitioners develop more effective, tailored interventions. To address this gap, we conducted a systematic review to identify the risk factors of depression among adolescents with NSSI that could be utilized to develop interventions that reduce risk factors leading to depression in NSSI.
Material and Methods
Search strategy
Searching was conducted across four databases, consisting of PubMed, CINAHL, ScienceDirect, and Scopus, from 2014 to 2024. Limiting the review to the past
decade ensures that our findings are based on the most up-to-date evidence. We performed a systematic review of the literature, which followed the preferred reporting items for systematic reviews and meta-analysis (PRISMA) guidelines outlined in (Page et al., 2021). We aimed to answer the PECO criteria to formulate a focused review question, “What are the risk factors for depression among adolescents with NSSI?” (Table 1).

All retrieved articles were imported into EndNote software, version 21 to identify relevant studies and remove duplicates. We used boolean operators (AND, OR, NOT, or AND NOT) as conjunctions to combine or exclude keywords in our searching (Table 2).

Eligibility criteria and study selection
The study population is adolescents with NSSI who are 10-21 years old and presented with depression (American Academy of Pediatrics, 2019). No specific intervention was required for inclusion in this review. Studies relevant to non-experimental designs, such as cross-sectional studies, published in English between 2014 and 2024, were included. However, studies were excluded if they were not available in full text, if the sample populations consisted of adults or older people, or if they were case studies, systematic reviews, or meta-analysis articles.
Data extraction and synthesis
Data extraction and cross-checking were conducted by two authors, who screened the articles by reviewing their design, participants, risk factors, measurements, and main findings to determine if they met the inclusion criteria. After this screening procedure, full-text articles were analyzed in detail for final inclusion, focusing on the relationship between depression and its associated factors. Data were summarized as adjusted odds ratios, and multivariate findings took precedence over unadjusted odds ratios and bivariate results. Any disagreements between the two authors were referred to a third author for a final decision. We conducted a narrative synthesis to identify risk factors of depression. We categorized findings of the included studies into three domains (biological, psychological, and sociological factors), enabling us to identify common risk factors for depression and inconsistencies across studies. To enhance clarity, we developed a summary table to present findings in a structured format.
Quality assessment
The quality of the studies was assessed by using the Joanna Briggs Institute (JBI) critical appraisal checklist (Moola et al., 2020) for cross-sectional studies. Studies scoring over 70% (6–8 points) were classified as high quality, those scoring between 50% and 70% (4–5 points) as medium quality, and those below 50% (below 4 points) as low quality (Moola et al., 2017).
Results
Following the selection process, 2457 articles were imported into EndNote software, to identify relevant articles and remove duplicates (1431 articles). This process left 1026 potentially relevant sources. Of these, 1007 articles were excluded for various reasons, such as lack of full text, not focusing on adolescents, or being related to other diseases. Finally, 19 articles were selected that satisfied the criteria set forth for this systematic review (Figure 1).
Study characteristics
Nineteen studies met the eligibility criteria. All of these were cross-sectional studies; 13 were conducted in China, 2 in the USA, and 1 study each in Canada, Germany, Belgium, and Turkey. The mean age of adolescent participants ranged from 13.05 to 18.73 years, although three studies did not report the mean age of participants. Additionally, ten studies focused on adolescents in hospital settings, while nine involved adolescents in school communities.
The adolescent’s depression had been measured using various measurements, including the Center for epidemiological studies depression scale (CES-D), depressive symptoms scale (DSS), the Beck depression inventory (BDI), the revised child anxiety and depression scale child version (RCADS-C), Hamilton depression scale (HAMD), the patient health questionnaire (PHQ), the depression-anxiety-stress scale (DASS), the children’s depression inventory (CDI), the hospital anxiety and depression scale (HADS), the Ko’s depression inventory (KDI), the diagnostic and statistical manual of mental disorders (DSM), and the international classification of diseases (ICD) (Table 3).


Risk of bias
The Joanna Briggs Institute (JBI) critical appraisal checklist for analytical cross-sectional studies was used to evaluate the methodological quality of eligible studies. This assessment checklist has 8 questions and sections to record answers as “yes,” “no,” “unclear,” or “not applicable” (Moola et al., 2017). All studies were classified as high quality. Of the 19 studies, most described the subjects and settings used valid and reliable measurements and applied appropriate statistical analyses to assess outcomes. However, one study did not describe valid and reliable measures, and six studies did not report confounding factors (Table 4).

Risk factors associated with depression among adolescents with NSSI
This study found that depression among adolescents with NSSI is influenced by multiple factors, including biological, psychological, and sociological factors (Table 5).


Biological factors
Biological factors encompass fundamental biomedical influences, including genetic predispositions, brain structure and function, and neurochemical imbalances, all of which play a significant role in the development of depression. However, these biological processes can be shaped or exacerbated by external factors such as infections, injuries, diet, exposure to toxins, or trauma, which may impact mental health (Karunamuni et al., 2021). For instance, genetic predispositions may interact with environmental stressors, such as childhood maltreatment or prolonged emotional trauma, increasing the risk of depression and NSSI. These factors can be further explained as follows.
Gender: Out of the 19 studies, two studies reported that being female increases the risk of depression in adolescents with NSSI (Baiden et al., 2017; Ren et al., 2024), while one study reported that being male increases the risk of depression (Cao et al., 2024).
Behavior of alcohol use: Out of the 19 studies, one study indicated that active drinking alcohol use increases the risk of depression (Cao et al., 2024).
Exposure to negative life events: Out of the 19 studies, one indicated that personal distress and stressful life events increased the risk of depression (Wei et al., 2022).
Psychological factors
Psychological factors refer to internal mental processes, emotions, attitudes, and beliefs that influence an individual’s behavior, thoughts, and decision-making (George, 2012). These factors, including coping mechanisms, personality traits, and emotional responses, influence how individuals interact with their environment and experiences. These factors can be explained as follows.
Mental health condition: Out of the 19 studies, four investigated the increased risk of depression among adolescents with borderline personality disorder (Chen et al., 2023a; Chen et al., 2023b; Ghinea et al., 2021; Lu et al., 2023), while two studies indicated that anxiety also raises the risk of depression (Hu et al., 2021; Luyckx et al., 2015). Additionally, one study found that alexithymia increases the risk of depression (Tang et al., 2022), and another found that hopelessness increases the risk of depression (Chen et al., 2023a).
Self-directed behaviors: Out of the 19 studies, two investigated that experiential avoidance increased the risk of depression (Ding et al., 2022; Hu et al., 2021), while two studies indicated that emotion dysregulation also raises the risk of depression (Ateş et al., 2024; Chen et al., 2023b). Additionally, two indicated that impulsiveness also increases the risk of depression (Liu et al., 2024; Ren et al., 2024), and another indicated that low self-compassion and self-punishment increase the risk of depression (Ateş et al., 2024).
Cognitive function: Out of the 19 studies, three investigated rumination through increased risk of depression, including brooding and dampening (Burke et al., 2018; Chen et al., 2023a; Luyckx et al., 2015), while one study reported cognitive impairment increased risk of depression (Hu et al., 2021).
Sociological factors
Sociological factors refer to the societal and environmental aspects that shape human behavior, beliefs, and interactions (George, 2012). These factors encompass social structures, cultural norms, and systemic elements, including family, religion, education, socioeconomic status, and community values. These factors can be explained as follows.
Education: Out of the 19 studies, one indicated that adolescents in junior high school or below have an increased risk of depression (Cao et al., 2024).
Cumulative ecological risk: Only one of the 19 studies examined cumulative ecological factors that predicted depression in adolescents with NSSI, including connections between parents and children, peers, and teachers and students (Liu et al., 2024).
Parent relationships: Out of the 19 studies, 5 studies reported that childhood maltreatment or childhood abuse increases the risk of depression (Baiden et al., 2017; Cao et al., 2024; Ghinea et al., 2021; Liu et al., 2024b; Wu et al., 2023). Additionally, one study indicated that caregiver divorce or family separation increases the risk of depression (Wang et al., 2024), and another indicated that interpersonal boundaries and function increase the risk of depression (Ateş et al., 2024).
Abuse/Trauma: Out of the 19 studies, two studies reported that physical and sexual abuse increase the risk of depression (Liu et al., 2024b; Wang et al., 2024). Additionally, one study investigated that emotional neglect increases the risk of depression (Wang et al., 2024), and another identified that emotional abuse and physical neglect increase the risk of depression (Liu et al., 2024b).
School bullying: Out of the 19 studies, three studies indicated that relationship bullying increases the risk of depression (Liu et al., 2024b; Vergara et al., 2019; Wang et al., 2024), while one study identified that cyber-ostracism increases the risk of depression (Ding et al., 2022). Additionally, one study investigated how verbal and physical bullying increases the risk of depression (Liu et al., 2024b).
Discussion
This systematic review explored risk factors associated with depression in adolescents who engage in NSSI. A total of 19 cross-sectional studies among 31058 adolescents with NSSI met the eligibility criteria. The findings indicated that depression risk is influenced by three key domains: Biological factors, including female gender, behavior of alcohol use, and exposure to negative life events; psychological factors, such as pre-existing mental health conditions, psychological distress, and cognitive functioning; and sociological factors, including educational background, parental relationships, experiences of abuse or trauma, and peer bullying. These findings highlight the multifaceted nature of depression risk in this population.
Biological factors
The literature reports that women, in particular, who engage in NSSI are more likely than men to have experienced depression (Baiden et al., 2017; Ren et al., 2024). However, one study reported that being male gender increases the risk of depression (Cao et al., 2024). The reason for the gender differences may be related to the fact that women generally have higher rates of depression and anxiety than men (Hilt et al., 2008). The average age of adolescent participants ranged from 13.05 to 18.73 years. The finding was consistent with the previous review by Cao et al. (2024), who indicated that adolescents in junior high school or below have an increased risk of depression. Similarly, Kessler et al. (2005) explained that mid-adolescent age is a predictor of NSSI across the lifespan, as adolescence is a critical period for human development in lifelong well-being. Still, the risk of poor mental health is found in 50% of all mental disorders beginning by age 14. Moreover, adolescents experiencing personal distress and stressful life events have an increased risk of depression (Ren et al., 2024; Wei et al., 2022). This finding is consistent with the findings of Baetens et al. (2021), who reported that the presence of depression in adolescents with NSSI is associated with an increased likelihood of experiencing stressful life events. Adolescents engaging in NSSI may be more susceptible to interpersonal conflicts, including arguments with parents, teachers, friends, or romantic partners. Additionally, these findings align with previous research suggesting that depression may serve as a mechanism linking stressful life events to NSSI in adolescents (Burke et al., 2015; Liu et al., 2021).
Psychological factors
This review found that psychological factors are strongly associated with depression in adolescents with NSSI, which is often used to regulate distressing emotions, manage stress, or self-punishment. It may also serve as an outlet for self-directed anger, self-blame, and perceived social transgressions (Chapman & Dixon-Gordon, 2007; Klonsky & Muehlenkamp, 2007). Additionally, mental health condition increases the risk of depression, such as borderline personality disorder, anxiety, alexithymia, and hopelessness (Chen et al., 2023a; Chen et al., 2023b; Ghinea et al., 2021; Hu et al., 2021; Lu et al., 2023; Luyckx et al., 2015; Tang et al., 2022). The findings align with previous studies that highlighted how depression among adolescents with NSSI may be linked to other mental health conditions, particularly in those who struggle with mood regulation (Andover & Gibb, 2010; Whitlock et al., 2014). NSSI is often carried out as an attempt to avoid interpersonal interactions. Individuals with mood disorders who engage in NSSI frequently have a history of poor or negative relationships, exhibit impulsiveness, and experience low self-compassion, which may also engage in self-punishment, as shown in previous findings.
Cognitive function, including rumination thought, brooding, dampening, and cognitive impairment, is associated with depression (Burke et al., 2018; Chen et al., 2023a; Hu et al., 2021; Luyckx et al., 2015). The response style theory developed by Nolen-Hoeksema (1991) explains that an individual’s response to distractions can lead to depression, particularly in those with a tendency to ruminate. Rumination involves repetitive, negative thoughts that prolong distress and increase the risk of depression more than in individuals who do not engage in such thinking patterns.
Sociological factors
The findings highlight cumulative ecological risks, including poor parent-child relationships, adverse family life events, academic challenges, teacher-student relationships, and peer relationships (Liu et al., 2024a). Sociological factors, including parent relationships, abuse, and school bullying, were identified as risk factors for depression. This systematic review indicates that childhood maltreatment or abuse, caregiver divorce or family separation, and interpersonal boundary issues increase the risk of depression (Ateş et al., 2024; Baiden et al., 2017; Cao et al., 2024; Ghinea et al., 2021; Liu et al., 2024b; Wang et al., 2024; Wu et al., 2023). This finding may be because childhood abuse is often associated with long-term emotional dysfunction. Adolescents with a history of childhood abuse tend to struggle with affect and emotion regulation and may experience a sense of insecurity, which can consequently lead to NSSI (Santangelo et al., 2016).
Moreover, being abused from childhood trauma such as physical abuse, sexual abuse, emotional abuse, emotional neglect, and physical neglect is a risk factor for depression (Liu et al., 2024b; Wang et al., 2024). It suggests that victims of sexual abuse often experience a profound sense of betrayal and depersonalization, which can lead to maladaptive strategies for regulating emotions in an attempt to reduce emotional distress (Lu et al., 2023). Moreover, physical abuse significantly affects adolescents with depression who engage in NSSI, as these adolescents often have limited emotion regulation skills. The negative emotions stemming from physical abuse may lead them to use NSSI as a quick way to regulate their emotions (Chapman & Dixon-Gordon, 2007). These findings confirm that a sense of loss and helplessness when witnessing caregivers being treated violently contribute to various mental health issues, such as depression, which were identified as predictors of NSSI.
School bullying by peers, such as relationship bullying, cyber-ostracism, and verbal and physical bullying, is found to be a risk factor for depression (Ding et al., 2022; Liu et al., 2024b; Wang et al., 2024). This finding suggests that experiencing school bullying can be a significant stressor that leads to an accumulation of depression, potentially resulting in self-injurious behavior as a form of emotional relief (Ford & Gómez, 2015). Similarly, adolescents who are victims of school bullying may experience depression and engage in self-harm as a coping mechanism or form of self-punishment (Nguyen et al., 2020).
This study has some limitations. The inclusion criteria are limited to English-language publications from 2014 to 2024, which may introduce selection bias. Furthermore, some studies did not provide the average age of participants, which could potentially impact the results, as adolescence is divided into three stages: Early, middle, and late adolescence, each with distinct developmental characteristics. Specifying the average age could help clarify which stage of adolescence is most associated with NSSI and an increased risk of developing depression. Moreover, the measurement of depression differed among studies, with some using a wide range of scores that might also include other disorders such as anxiety and stress. This may lead to variability in measuring depression due to the influence of comorbid conditions.
Conclusion
The findings are classified into three categories of factors associated with depression among adolescents with NSSI. These are biological factors, consisting of gender, behavior of alcohol use, and exposure to negative life events; psychological factors, consisting of mental health conditions, psychological behaviors, and cognitive function; and sociological factors, consisting of education, parent relationships, experiences of abuse or trauma, and school bullying.
Ethical Considerations
Compliance with ethical guidelines
The study protocol was registered with the international prospective register of systematic reviews (PROSPERO) (Code: CRD42024555723).
Funding
This study was extracted from the PhD dissertation of Russunan Jantarapakdee, approved by the Faculty of Nursing at Chulalongkorn University, Bangkok, Thailand. This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Investigation, data collection, and validation: Russunan Jantarapakdee and Ratchaneekorn Upasen; Data analysis and writing: Russunan Jantarapakdee and Penpaktr Uthis; Final approval: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors want to express their gratitude to the Faculty of Nursing, Chulalongkorn University and the Faculty of Nursing, Burapha University for providing their constant support for the study.
References
American Academy of Pediatrics., 2019. Stages of adolescence. Illinois: American Academy of Pediatrics. [Link]
Andover, M. S. & Gibb, B. E., 2010. Non-suicidal self-injury, attempted suicide, and suicidal intent among psychiatric inpatients. Psychiatry Research, 178(1), pp. 101-5. [DOI:10.1016/j.psychres.2010.03.019] [PMID]
Asarnow, J. R., et al., 2011. Suicide attempts and nonsuicidal self-injury in the treatment of resistant depression in adolescents: Findings from the TORDIA study. Journal of the American Academy of Child and Adolescent Psychiatry, 50(8), pp. 772–81.[DOI:10.1016/j.jaac.2011.04.003] [PMID]
Ateş, B. Ö., et al., 2024. Self-compassion and psychological mindedness in depressed Turkish adolescents with non-suicidal self-injury. Australian Psychologist, 59(5), pp. 435-48. [DOI:10.1080/00050067.2024.2371802]
Baetens, I., et al., 2021. Predictors and consequences of non-suicidal self-injury in relation to life, peer, and school factors. Journal of Adolescence, 90, pp. 100–8. [DOI:10.1016/j.adolescence.2021.06.005] [PMID]
Baiden, P., Stewart, S. L. & Fallon, B., 2017. The mediating effect of depressive symptoms on the relationship between bullying victimization and non-suicidal self-injury among adolescents: Findings from community and inpatient mental health settings in Ontario, Canada. Psychiatry Research, 255, pp. 238–47. [DOI:10.1016/j.psychres.2017.05.018] [PMID]
Barrocas, A. L., et al., 2015. Nonsuicidal self-injury in adolescence: Longitudinal course, trajectories, and intrapersonal predictors. Journal of Abnormal Child Psychology, 43(2), pp. 369–80. [DOI:10.1007/s10802-014-9895-4] [PMID]
Bousoño, M., et al., 2021. Alcohol use and risk factors for self-harm behavior in Spanish adolescents. Adicciones, 33(1), pp. 53–62. [DOI:10.20882/adicciones.1239] [PMID]
Bronfenbrenner, U., 2005. Making human beings human: Bioecological perspectives on human development. California: SAGE. [Link]
Brown, R. C. & Plener, P. L., 2017. Non-suicidal Self-Injury in Adolescence. Current Psychiatry Reports, 19(3), pp. 20. [DOI:10.1007/s11920-017-0767-9] [PMID]
Burke, T. A., et al., 2018. Latent classes of trait affect and cognitive affective regulation strategies are associated with depression, non-suicidal self-injury, and well-being. Journal of Affective Disorders, 225, pp. 180–7. [DOI:10.1016/j.jad.2017.08.015] [PMID]
Burke, T. A., et al., 2015. Non-suicidal self-injury prospectively predicts interpersonal stressful life events and depressive symptoms among adolescent girls. Psychiatry Research, 228(3), pp.416–24. [DOI:10.1016/j.psychres.2015.06.021] [PMID]
Cao, P., et al., 2024. Predictors of non-suicidal self-injury in adolescents with depressive disorder: the role of alexithymia, childhood trauma, and body investment. Frontiers in Psychology, 15, pp. 1336631. [DOI:10.3389/fpsyg.2024.1336631] [PMID]
Chapman, A. & Dixon-Gordon, K., 2007. Emotional antecedents and consequences of deliberate self-harm and suicide attempts. Suicide & Life-Threatening Behavior, 37(5), pp. 543–52. [DOI:10.1521/suli.2007.37.5.543] [PMID]
Chen, H., et al., 2023. Cognitive impairment and factors influencing depression in adolescents with suicidal and self-injury behaviors: A cross-sectional study. BMC Psychiatry, 23(1), pp. 247. [DOI:10.1186/s12888-023-04726-8] [PMID]
Chen, Y., et al., 2023. Relationship between borderline personality features, emotion regulation, and non-suicidal self-injury in depressed adolescents: A cross-sectional study. BMC Psychiatry, 23(1), pp. 293. [DOI:10.1186/s12888-023-04800-1] [PMID]
Claes, L., et al., 2010. Comparison of non-suicidal self-injurious behavior and suicide attempts in patients admitted to a psychiatric crisis unit. Personality and Individual Differences, 48(1), pp. 83-7. [DOI:10.1016/j.paid.2009.09.001]
Ding, H., et al., 2022. The relationship between cyber-ostracism and adolescents’ non-suicidal self-injury: Mediating roles of depression and experiential avoidance. International Journal of Environmental Research and Public Health, 19(19), pp. 12236. [DOI:10.3390/ijerph191912236] [PMID]
Du, N., et al., 2021. Psychosocial factors associated with increased adolescent non-suicidal self-injury during the covid-19 pandemic. Frontiers in Psychiatry, 12, pp. 743526. [DOI:10.3389/fpsyt.2021.743526] [PMID]
Esposito, C., et al., 2023. Prevalence of engagement and frequency of non-suicidal self-injury behaviors in adolescence: An investigation of the longitudinal course and the role of temperamental effortful control. European Child & Adolescent Psychiatry, 32(12), pp. 2399–414. [DOI:10.1007/s00787-022-02083-7] [PMID]
Ford, J. D. & Gómez, J. M., 2015. The relationship of psychological trauma and dissociative and posttraumatic stress disorders to nonsuicidal self-injury and suicidality: A review. Journal of Trauma & Dissociation: The Official Journal of the International Society for the Study of Dissociation (ISSD), 16(3), pp. 232–71. [DOI:10.1080/15299732.2015.989563] [PMID]
George, L. E., 2012. The need for a new medical model: A challenge for biomedicine. Psychodynamic Psychiatry, 40(3), pp. 377-96. [DOI:10.1521/pdps.2012.40.3.377] [PMID]
Ghinea, D., et al., 2021. Psychosocial functioning in adolescents with non-suicidal self-injury: the roles of childhood maltreatment, borderline personality disorder and depression. Borderline Personality Disorder and Emotion Dysregulation, 8(1), pp. 21. [DOI:10.1186/s40479-021-00161-x] [PMID]
Gillies, D., et al., 2018. Prevalence and characteristics of self-harm in adolescents: Meta-Analyses of community-based studies 1990-2015. Journal of the American Academy of Child and Adolescent Psychiatry, 57(10), pp. 733–41. [DOI:10.1016/j.jaac.2018.06.018] [PMID]
Hilt, L. M., Cha, C. B. & Nolen-Hoeksema, S., 2008. Nonsuicidal self-injury in young adolescent girls: Moderators of the distress-function relationship. Journal of Consulting and Clinical Psychology, 76(1), pp. 63–71. [DOI:10.1037/0022-006X.76.1.63] [PMID]
Hu, Z., et al., 2021. Relationship among self-injury, experiential avoidance, cognitive fusion, anxiety, and depression in Chinese adolescent patients with nonsuicidal self-injury. Brain and Behavior, 11(12), pp. e2419. [DOI:10.1002/brb3.2419] [PMID]
Jin, M. K., et al., 2023. A systematic review and meta-analysis of factors related to non-suicidal self-injury among Chinese adolescents. Psychiatry Research, 326, pp. 115329. [DOI:10.1016/j.psychres.2023.115329] [PMID]
Kabkumba, C., Kaewjanta, N., & Rungreangkulkij, S. (2021). Non-suicidal self-harm behaviour and risk factors amongst undergraduate nursing students. Journal of Thailand Nursing and Midwifery Council 37(1), 146-160. [Link]
Karunamuni, N., Imayama, I. & Goonetilleke, D., 2021. Pathways to well-being: Untangling the causal relationships among biopsychosocial variables. Social Science & Medicine (1982), 272, pp. 112846. [DOI:10.1016/j.socscimed.2020.112846] [PMID]
Kerr, P. L., Muehlenkamp, J. J. & Turner, J. M., 2010. Nonsuicidal self-injury: A review of current research for family medicine and primary care physicians. Journal of the American Board of Family Medicine: JABFM, 23(2), pp. 240–59. [DOI:10.3122/jabfm.2010.02.090110] [PMID]
Kessler, R. C., et al., 2005. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry, 62(6), pp. 593-602. [DOI:10.1001/archpsyc.62.6.593] [PMID]
Klonsky, E. D. & Muehlenkamp, J. J., 2007. Self-injury: A research review for the practitioner. Journal of Clinical Psychology, 63(11), pp. 1045–56. [DOI:10.1002/jclp.20412] [PMID]
Lawrence, D., et al., 2016. Key findings from the second Australian Child and Adolescent Survey of Mental Health and Wellbeing. The Australian and New Zealand Journal of Psychiatry, 50(9), pp. 876–86. [DOI:10.1177/0004867415617836] [PMID]
Liu, S., et al., 2024. Cumulative ecological risk and nonsuicidal self-injury in adolescents: The mediation of depression and the moderation of impulsiveness. Child: Care, Health and Development, 50(1), pp. e13211. [DOI:10.1111/cch.13211] [PMID]
Liu, Y., et al., 2024. The mediating effects of school bullying victimization in the relationship between childhood trauma and NSSI among adolescents with mood disorders. BMC Pediatrics, 24(1), pp. 524. [DOI:10.1186/s12887-024-04986-7] [PMID]
Liu, Z. Z., et al., 2021. Depression as a mediator between frequent nightmares and non-suicidal self-injury among adolescents: A 3-wave longitudinal model. Sleep Medicine, 77, pp. 29–34. [DOI:10.1016/j.sleep.2020.11.015] [PMID]
Lu, Z., et al., 2023. The relationship between depressive mood and non-suicidal self-injury among secondary vocational school students: The moderating role of borderline personality disorder tendencies. Frontiers in Psychiatry, 14, pp. 1187800.[DOI:10.3389/fpsyt.2023.1187800] [PMID]
Luyckx, K., et al., 2015. Non-suicidal self-injury in high school students: Associations with identity processes and statuses. Journal of Adolescence, 41, pp.76–85. [DOI:10.1016/j.adolescence.2015.03.003] [PMID]
Moola S, et al., 2017. Chapter 7: Systematic reviews of etiology and risk. In: Aromataris E, Munn Z (Editors). Checklist for analytical. Cross sectional studies. North Adelaide: The Joanna Briggs Institute. [Link]
Moola, S., et al., 2020. Systematic reviews of etiology and risk.In: E. Aromataris & Z. Munn (Editors). JBI Manual for Evidence Synthesis. Adelaide: JBI. [Link]
Muehlenkamp, J. J. & Brausch, A. M., 2019. Protective factors do not moderate risk for past-year suicide attempts conferred by recent NSSI. Journal of Affective Disorders, 245, pp. 321–4. [DOI:10.1016/j.jad.2018.11.013] [PMID]
Nguyen, H. T. L., et al., 2020. Relationships among cyberbullying, parental attitudes, self-harm and suicidal behavior among adolescents: Results from a school-based survey in Vietnam. BMC Public Health, 20(1), pp. 476. [DOI:10.1186/s12889-020-08500-3] [PMID]
Nolen-Hoeksema, S., 1991. Responses to depression and their effects on the duration of depressive episodes. Journal of Abnormal Psychology, 100(4), pp. 569–82. [DOI:10.1037/0021-843X.100.4.569] [PMID]
Page, M. J., et al., 2021. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ (Clinical research ed.), 372, pp. n71. [PMID]
Ren, T., et al., 2024. Psychosocial factors affect the occurrence of nonsuicidal self-injury in adolescents with major depressive disorder through chain mediation. European Archives of Psychiatry and Clinical Neuroscience, 275(4), pp. 1209–20.[DOI:10.1007/s00406-024-01858-0] [PMID]
Santangelo, P. S., et al., 2017. Ecological momentary assessment of affective and interpersonal instability in adolescent non-suicidal self-injury. Journal of Abnormal Child Psychology, 45(7), pp. 1429–38. [DOI:10.1007/s10802-016-0249-2] [PMID]
Shao, C., et al., 2021. Analysis of risk factors of non-suicidal self-harm behavior in adolescents with depression. Annals of Palliative Medicine, 10(9), pp. 9607–13. [DOI:10.21037/apm-21-1951] [PMID]
Tang, W. C., et al., 2022. Mediating role of depression in the association between alexithymia and nonsuicidal self-injury in a representative sample of adolescents in Taiwan. Child and Adolescent Psychiatry and Mental Health, 16(1), pp. 43. [DOI:10.1186/s13034-022-00477-8] [PMID]
Thai, T. T., et al., 2021.The prevalence, correlates and functions of non-suicidal self-injury in Vietnamese adolescents. Psychology Research and Behavior Management, 14, pp. 1915–27. [DOI:10.2147/PRBM.S339168] [PMID]
Vergara, G. A., et al., 2019. Non-Suicidal self-injury and suicide in depressed Adolescents: Impact of peer victimization and bullying. Journal of Affective Disorders, 245, pp. 744–9. [DOI:10.1016/j.jad.2018.11.084] [PMID]
Wang, L., et al., 2024. Prevalence of adverse childhood experiences and their associations with non-suicidal self-injury among Chinese adolescents with depression. Child Psychiatry and Human Development, 55(5), pp. 1441–51. [DOI:10.1007/s10578-023-01508-x] [PMID]
Wang, Y. J., et al., 2022. Risk factors for non-suicidal self-injury (NSSI) in adolescents: A meta-analysis. EClinicalMedicine, 46, pp. 101350. [DOI:10.1016/j.eclinm.2022.101350] [PMID]
Wei, C., et al., 2022. Stressful life events and non-suicidal self-injury among Chinese adolescents: A moderated mediation model of depression and resilience. Frontiers in Public Health, 10, pp. 944726. [DOI:10.3389/fpubh.2022.944726] [PMID]
Whitlock, J., Exner-Cortens, D. & Purington, A., 2014. Assessment of nonsuicidal self-injury: Development and initial validation of the Non-Suicidal Self-Injury-Assessment Tool (NSSIAT). Psychological Assessment, 26(3), pp. 935–46. [DOI:10.1037/a0036611] [PMID]
Wu, J., et al., 2023. The effects of childhood abuse, depression, and self-compassion on adolescent nonsuicidal self-injury: A moderated mediation model. Child Abuse & Neglect, 136, pp. 105993. [DOI:10.1016/j.chiabu.2022.105993] [PMID]
Yu, L., et al., 2023. Multicenter analysis on the non-suicidal self-injury behaviors and related influencing factors-A case study of left-behind children in northeastern Sichuan. Journal of Affective Disorders, 320, pp. 161–8. [DOI:10.1016/j.jad.2022.09.081] [PMID]
Type of Study: Review Article |
Subject:
Special
Received: 2024/12/17 | Accepted: 2025/04/12 | Published: 2025/11/1
Received: 2024/12/17 | Accepted: 2025/04/12 | Published: 2025/11/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |







